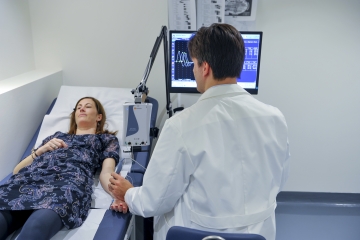
What is ENMG?
Electroneuromyography is the functional exploration of the peripheral nervous system. It is a functional examination, i.e. an examination that makes it possible to test the nerves and muscles in vivo, meaning that no imaging examination, such as scanning or MRI, is involved.
The test is usually performed in two parts, the first being stimulus detection. This involves an analysis of nervous, sensitive and motor inputs. It takes the form of tiny electrical stimulations of the upper and/or lower limbs or of the face, the responses being collected through electrodes arranged on the surface that stimulates voluntary electrical activity emanating from the brain.
Sensitive neurography:
The nerve is stimulated and the nerve’s response or potential is recorded. The nerves most frequently examined in the upper limbs are the median, cubital and radial nerves and those most frequently examined in the lower limbs are the sural and proximal peroneal nerves. This analysis relates to the speed of nerve conduction, the amplitude of potential, reflecting the number of fibres within the nerves concerned, and its duration.
Motor neurography:
The nerve is stimulated and the muscle response or potential is recorded. The nerves most frequently examined in the upper limbs are the median, ulnar and radial nerves and those in the lower limbs are the common fibular nerves, the tibial nerve and the femoral nerve. The facial nerve is examined in cases of facial paralysis. Measurements are taken of the distal latency, the speed of nerve conduction, the amplitude of nerve potential and its duration.
Myography:
The second part is known as myography, or a detection examination, involving an analysis of electrical activity in the muscles tested. This exploratory procedure is performed using a disposable fine sterile needle, connected to an amplifier and a computer; this enables analysis of the muscles when resting and under strain. Specific anomalies can be recorded, such as resting potential (fibrillation and positive potential) or fasciculation. When muscles are exercised, normal tracing is known as interferential. Neurogenic or myogenic activity may be detected, depending on the type of damage. In this case, there is no electrical stimulation.
Electrical stimulations can sometimes be perceived as unpleasant, but such sensations last only a short time (tenths of milliseconds) and present no danger of electrocution or nerve degeneration, since the apparatus is insulated and earthed.
ENMG can be used for a wide variety of indications, and makes it possible to investigate the spinal cord neurons and the nerve fibres that emerges from it (roots, plexus, nerves) as well as the neuro-muscular junction and the muscles themselves. The symptomatology giving rise to an ENMG is very diverse, and can include sensory disruption (formication, numbness, loss of sensitivity, pain of the electrical discharge type), motor disorders (lack of strength, cramps, atrophy, spontaneous muscle movements (myokymia, fasciculation) and over- or under-active reflexes (hypo- or hyper-reflexia).
As a general rule, any damage to the peripheral, focal or diffuse nervous system, any muscle disturbance or disruption to the nerve-muscle junction is a reason for an ENMG to be performed. There is no protocol or standardisation for this examination, and the way in which it is performed depends upon the prior clinical assessment conducted by the doctor. The sequence for the conduct of the examination is always explained to the patient. The examination normally lasts between 30 and 60 minutes, depending upon the type of disorder.
Contraindications are rare. Therapeutic anticoagulation treatment or a problem with blood coagulation can restrict a myographical examination, but not nerve stimulations. A pacemaker implanted in the heart will restrict very proximal stimulation, but not the remainder of the examination.
A few practical examples are set out below, although naturally this is not an exhaustive list:
-
Carpal tunnel syndrome is a condition that typically manifests itself through sensory disturbance (formication/numbness) in the hands and/or a loss of strength. The condition is due to compression of the median nerve in the wrist (the carpal tunnel) for which there are a variety of causes. The examination makes it possible to confirm that the condition involves genuine compression of the median nerve, that it really does originate from the wrist, and permits the type of damage to be assessed (the myelin sheath around the nerve or damage to the nerve fibres themselves, known as axons) and the severity of the attack to be determined, together with its development. This makes it possible to decide whether treatment should be conservation (splint for the wrist) or surgical.
-
Ulnar nerve entrapment at the elbow also represents very frequent focal nerve damage. It often manifests as formication or loss of sensitivity in the last two fingers of the hand and/or loss of strength, due to irritation or compression of the nerve in its tunnel in the elbow. An examination makes it possible to specify the type of damage in question (whether to the sheath or the nerve fibre), to quantify the amount of damage, and to determine whether the damage is active or chronic.
-
Radial neuropathy of the arm or Saturday night’s palsy
-
Neuropathy of the common fibular nerve at the peroneal neck of the fibular
-
Meralgia parathestica
-
Damage to the facial nerve, determining the recovery prognosis
-
Cervicobrachialgia or lombar sciatalgia are common reasons for consultation. These conditions present respectively as pain in the back of the neck or the back, spreading distally, with or without the loss of muscle strength. Imaging often reveals degenerative disorders such as a narrow tunnel, arthrosis and discal hernia, whether or not in contact with various nerve roots. In such a case, an ENMG makes it possible to confirm or exclude an attack on a single root or multiple roots, to quantify the loss of nerve fibres and to determine whether the condition is active or chronic. In some cases, the attack is clinically evident, even though the ENMG is normal. In such cases, the attack is purely an irritation, making it possible to decide on the best treatment, whether conservation or surgical.
-
Characterisation and quantification of a polyneuropathy, permitting an etiological diagnosis
-
Diagnosis of acute or chronic polyradiculopathy (such as Guillain-Barré, CIDP)
-
Diagnosis and monitoring of problems in the neuromuscular junction, such as myasthenia
-
Assessment of conditions affecting the muscles (various myopathies or myositis)